The U.S. Challenge Around Herd Immunity
Herd immunity has become a household phrase in the U.S., yet few concepts are as misunderstood, controversial, or critical to our national health conversation. From pediatrician offices to school board meetings and public health briefings, Americans debate the meaning, limits, and practical realities of herd immunity against infectious diseases like measles, COVID-19, and polio.
Here’s the core problem: Although U.S. vaccines remain among the safest and most effective globally, declining immunization rates, rising vaccine hesitancy, misinformation, and policy shifts—such as some states reconsidering childhood vaccine mandates—threaten the ability of communities to achieve or maintain herd immunity. This has real consequences. Outbreaks of preventable diseases like measles resurge in regions where the “herd” is no longer sufficiently immune.
For parents, educators, and at-risk groups (including newborns, pregnant people, and the immunocompromised), confusion reigns: What does herd immunity really mean? How many people need to be immunized? Are vaccines alone enough? What diseases are most affected? U.S. communities face pragmatic decisions about vaccine uptake, public health, and social
responsibility.
The solution? Empower Americans with science-backed, accessible knowledge—explaining what herd immunity truly is, how it’s achieved, and why the right percentage of protection is everyone’s business. This ultimately bolsters public health, protects the most vulnerable, and prevents the avoidable return of once-defeated diseases.
What is Herd Immunity? Definitions, Synonyms, and U.S. Usage
Herd Immunity Definition and Synonyms
Herd immunity—sometimes called community immunity, population immunity, mass immunity, or the herd effect—describes a form of indirect protection from contagious infectious diseases. It occurs when a significant proportion of a population becomes immune, either through thorough vaccination or previous infection, thus hindering the spread of disease from person to person.
● Key synonyms: Community immunity, population immunity, mass immunity, herd effect. This means even those who are not immune (due to age, medical reasons, or choice) are less likely to be exposed—because the chains of infection are interrupted.
Herd immunity only works for diseases that spread from human to human (or animal to animal), not for those with environmental, non-human, or vector-reservoir transmission, nor for diseases that do not confer lasting immunity.
Why It Matters to the U.S. Public
In the American context, herd immunity forms the explicit rationale for childhood vaccine mandates in schools, outbreak control responses, and protection of the medically vulnerable.
When a community falls below the needed immunity threshold, it is not just an abstract problem: it means children, grandparents, and immunocompromised people face new risks from once-vanquished infections.
Direct quote from the CDC:
“Communities need to maintain high rates of vaccination to prevent outbreaks of disease and achieve what’s called herd immunity…herd immunity helps protect vulnerable members of the population who can’t get vaccinated, like those who are too young or immunocompromised.” CDC: Vaccines & Immunizations
How Herd Immunity Works: Mechanism and Disease Control
The Science and Mechanisms at Work
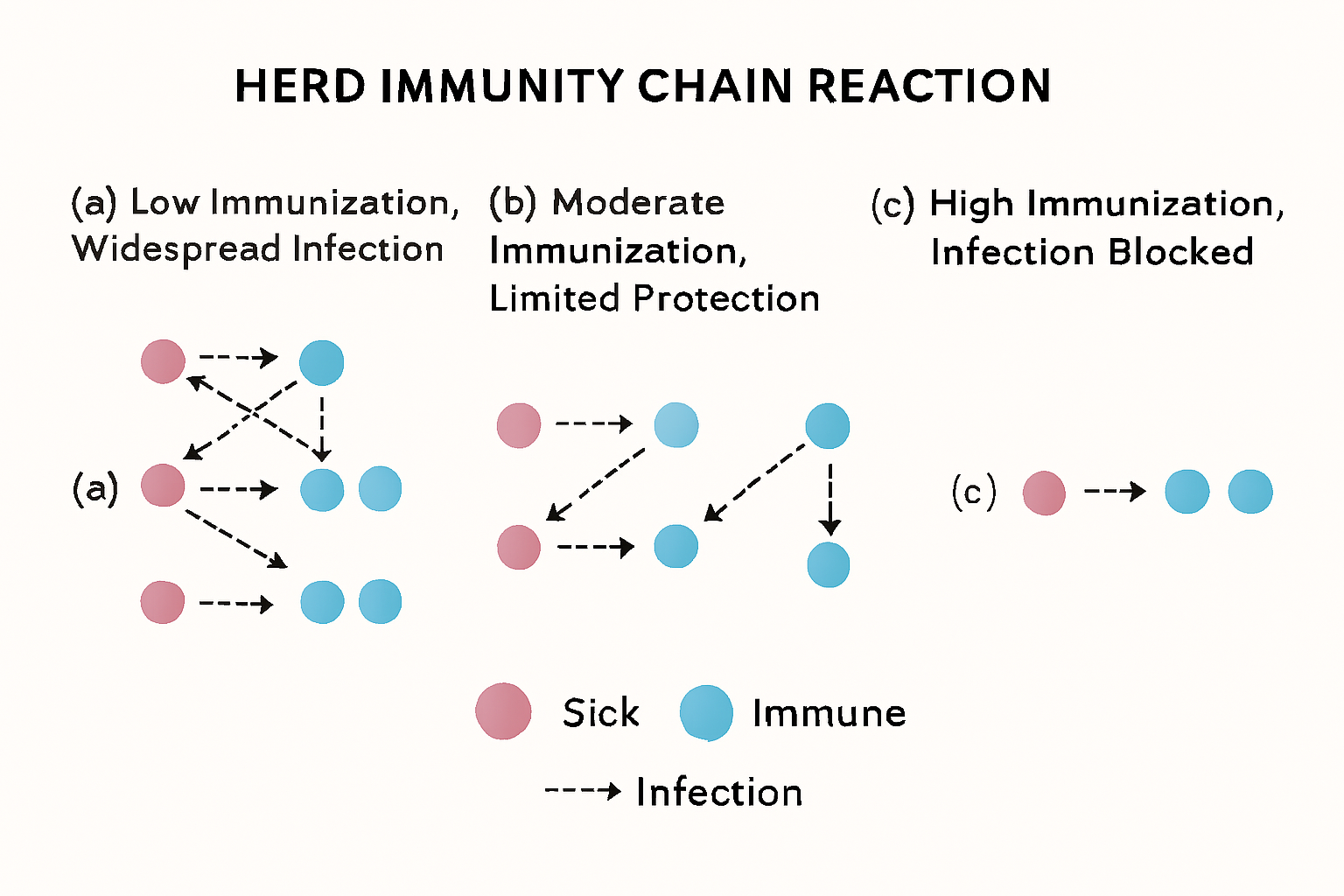
Herd immunity operates by breaking the chains of transmission. When most people in a community are immune, an infected individual has fewer susceptible people to infect. Disease outbreaks fizzle, and transmission becomes sporadic or stops altogether.
Main mechanism steps:
● Immunized individuals act as barriers—they either do not get infected upon exposure or, if infected, their immune system quickly contains and eliminates the pathogen, preventing onward transmission.
● Fewer susceptible hosts means the effective reproductive rate (the average number of people one infected person passes the disease to) falls below 1, causing outbreaks to dwindle.
Key Groups Protected by Herd Immunity
● Newborns and infants: Too young for full immunization schedules.
● Immunocompromised adults/children: e.g., cancer patients, transplant recipients, people with HIV, those on immunosuppressing medication.
● People allergic to vaccine components or with medical contraindications.
These individuals rely on the “herd” around them for their safety when vaccines do not work for them or aren’t allowed.
Ways Immunity Develops
There are two ways immunity can develop in the population:
- Vaccination: The safest and most controlled method, as it triggers the immune response without the risks of the actual disease.
- Natural infection: Recovery from the illness itself—often associated with unnecessary suffering, hospitalizations, deaths, or long-term complications. Not ethical or practical for serious diseases.
Cell-Level Safeguards: How the Immune System Knows Friend from Foe
Scientists wanted to figure out how this enzyme is regulated. They wanted to understand how the enzyme could trigger a strong response to foreign DNA from infections without causing a response against our own DNA. - That’s because if the enzyme comes into contact with our own DNA, it can trigger autoimmune diseases. “It’s a double-edged sword,” Dr. Chen says. “We need it to defend against infection, but if it’s improperly triggered by our own DNA, it can cause these autoimmune and inflammatory diseases.”
- The scientists designed a new study. In their research, they discovered something interesting – a tiny amount of either DNA or the enzyme fails to trigger a response. But when the enzyme and the DNA reach a certain concentration, the enzyme triggers the formation of special droplets.
- “Within this concentrated droplet, the enzyme becomes activated,” Dr. Chen says. The droplet acts like a microreactor within the cell, accelerating the enzyme to trigger the immune response. “It speeds up the reactions that churn out the small molecule cGAMP, which activates the immune system.” By EPA: Children’s Health and Vaccination
Public health consensus: Achieving herd immunity via widespread infection is not ethical—vaccines are the preferred route.
Calculating the Herd Immunity Threshold: Equations and Real Percentages
Understanding R₀ and Formulas
Basic Reproduction Number (R₀)
● R₀ (“R naught”) is the average number of people one infected person transmits the disease to in a totally susceptible population.
● Higher R₀ = harder to control, higher immunity threshold needed.
Herd Immunity Threshold (HIT) Equation
The proportion of the population that must be immune to stop sustained transmission is given by:
HIT = 1 – (1 / R₀)
Example calculations:
● If R₀ = 2: HIT = 1 – 1/2 = 0.5, or 50%
● If R₀ = 15 (measles): HIT = 1 – 1/15 = 0.93, or 93%
“For measles, R₀ ranges from 12–18, so at least 92–94% immunity is required for herd
immunity.”
Real-World Examples and Case Studies
Measles: The Classic Test Case
The U.S. Story: Measles was declared eliminated in the United States in 2000, thanks to widespread vaccination and herd immunity. - Yet, since 2019, clusters of unvaccinated people and slipping vaccine rates have led to the most measles cases in 30 years—with 1,356 cases across 40 states so far in 2025.
Key facts:
● Measles R₀: 12–18 (likely the most infectious virus known).
● Herd immunity threshold: 95% vaccination required.
● Current U.S. MMR coverage: 92.5% for kindergarteners (down from previous years; not high enough in many communities).
● Implications: Outbreaks in schools and communities occur when vaccine coverage falls even slightly below the threshold, especially in communities with clustered non-vaccination.
Simulation evidence:
Agent-based models at U.S. universities show dramatic differences in community measles outbreaks when vaccination drops to 80% versus 95%.
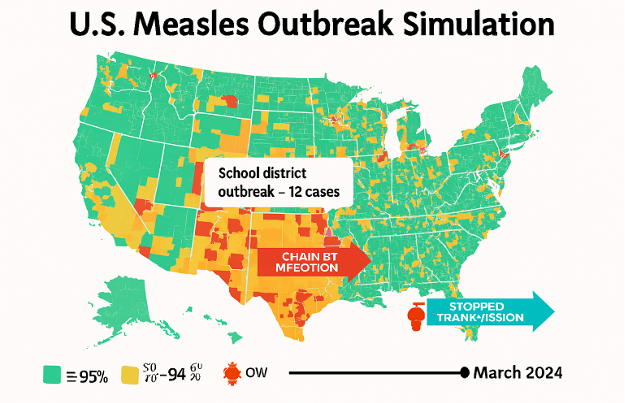
Key Point: Measles resurgence is not a theory, but an observed U.S. reality when the herd immunity threshold is missed, affecting mostly unvaccinated children and vulnerable individuals.
Polio: Lessons from the Past and the Threat of Return
● U.S. polio elimination: Achieved in 1979.
● Vaccine threshold: About 80–86% (with high effectiveness).
● Recent concern: Isolated cases in under-immunized U.S. communities (e.g., 2022 New York) show that even eradicated viruses can return if herd immunity slips due to vaccine refusals or waning immunity.
Other Successful Examples: Smallpox and Beyond
● Smallpox: The only human disease eradicated worldwide, using global vaccination and herd immunity, was declared eradicated in 1980.
● Rinderpest: Eradicated from cattle via vaccination.
Key lesson: High, sustained vaccine coverage using herd immunity can eliminate diseases, but loss of coverage risks re-emergence—even decades after supposed “elimination”.
The Role of Vaccines in Herd Immunity
How Vaccines Enable Herd Immunity
Vaccines mimic natural infection, but without the suffering or risk. They stimulate the immune system to produce memory cells and antibodies, so if the real disease is encountered, a prompt and strong defense is ready.By PAHO: Americas Immunization Program
Key Points:
● Higher vaccine coverage = stronger community protection. Most U.S. vaccines are highly effective, so high coverage equates to high immunity.
● Indirect protection: Vaccinated people don’t act as “spreader links,” reducing the chance of infection reaching susceptible people.
● Vaccinating specific age groups can protect others. Example: U.S. adults with pertussis boosters lowering infections in infants.
● Vaccines also block transmission (not just clinical disease). For herd immunity, a vaccine must disrupt person-to-person spread.
Vaccine Hesitancy and Public Health
The free rider problem: Some people who refuse vaccines benefit from the community’s protection, but as that group grows, outbreaks become inevitable and more severe for everyone—including the unvaccinated.
Reasons for hesitancy in the U.S. include:
● Misinformation about vaccine safety
● Distrust in institutions
● Political polarization
● Religious or personal beliefs
● Perceived low risk (due to prior success of herd immunity)
When hesitancy drives rates below the threshold, outbreaks harm those who opted out, but also babies, medically exempt, and others unable to immunize.
Reality Checks: Challenges, Limitations, and the “Herd Effect”
Difference Between Herd Immunity and Herd Effect
● Herd immunity: The theory (and sometimes reality) where enough immunity stops sustained transmission at the population level.
● Herd effect: Any reduction in disease in a community thanks to indirect protection, even if the threshold for full “herd immunity” isn’t reached.
Sometimes, vaccination campaigns create enough “herd effect” to meaningfully cut cases, but until the true threshold is achieved, outbreaks can still happen.
Barriers and Limitations in the U.S. Context
● Waning immunity: For some vaccines (like pertussis) or diseases (like COVID-19), immunity decreases, eroding protection without booster doses.
● Non-uniform coverage: Pockets of under-immunized communities can become outbreak epicenters—even if the overall state/national coverage is sufficient.
● Changing viruses: Flu and COVID-19 mutate, requiring updated vaccines and making population-level immunity a moving target.
● Population turnover: Newborns and migrants constantly add new susceptibles.
● Practicality: It is rarely feasible to immunize every individual—hence, herd immunity is vital for the unvaccinated and medically ineligible.By American Academy of Pediatrics: Immunization
The Reality for Emerging Diseases
COVID-19 lessons:
Initially, experts thought 60–70% population immunity (natural or vaccine-induced) might deliver herd immunity. Increased transmissibility of new variants, waning immunity, and uneven global vaccine access meant herd immunity was elusive for COVID-19—but vaccines still drastically reduced illness and deaths.
For future pandemics, these realities highlight both the potential and pitfalls of relying on herd immunity as a public health strategy.By EPA: Children’s Health and Vaccination
U.S. FAQs About Herd Immunity
What is the basic definition of herd immunity?
Direct answer for featured snippet:
Herd immunity is when a significant portion of a population becomes immune to an infectious disease—either via vaccination or previous infection—making it hard for the disease to spread. This indirectly protects those who are not immune.
How is the herd immunity threshold (HIT) calculated?
The threshold is calculated as 1 – (1 / R₀), where R₀ is the pathogen’s basic reproduction number. For example, for measles (R₀ = 15), the threshold is 1 – 1/15 = 0.93, or 93% immunity needed.
What diseases depend most on herd immunity?
Diseases that transmit directly from person to person and cause lasting immunity benefit most, such as measles, mumps, rubella, polio, and pertussis. Influenza and COVID-19 are more difficult due to viral mutation and waning immunity.
Can the U.S. achieve herd immunity without vaccines?
No, relying solely on natural infection for herd immunity would result in unnecessary deaths and overwhelmed hospitals. Vaccination is the only responsible, ethical route for diseases with high mortality or serious complications.
Is herd immunity equally protective everywhere?
Not necessarily. Pockets of low vaccination (e.g., “anti-vax” or underserved communities) experience outbreaks, even if statewide or national immunity is high. Risk is concentrated wherever the threshold is not met locally.
What is the difference between herd immunity and the herd effect?
Herd immunity is the theoretical threshold at which ongoing outbreaks stop; the herd effect is any population-level benefit from immunization, even if the threshold isn’t reached.
So, some reduction in transmission can occur before full herd immunity is achieved.
.
Key solution:
● Advocate for accurate vaccination information.
● Fight misinformation in your community.
● Ensure your family is up to date with recommended vaccines (consult your healthcare
provider).
● Support school, workplace, and healthcare immunization policies.
Together, we can keep diseases like measles, polio, and rubella rare, and shield those among
us who depend on the herd to stay healthy.
Want to protect your family and community?
● Speak to your doctor about recommended vaccines for your age group.
● Share this article with parents, school groups, and local leaders.
● Visit our pages on Vaccine Safety Myths and Facts and Family Outbreak Protection for
more resources. USDA: Public Health and Immunization
FAQs: Quick Answers to Your Top Herd Immunity Questions
What is herd immunity?
Herd immunity is when enough people have immunity (from vaccination or previous infection) that a disease can’t spread easily, thus protecting even those who aren’t immune.
How is herd immunity achieved?
Primarily through widespread vaccination, natural infection is not considered a safe or ethical
strategy for serious diseases.
Why do measles outbreaks happen in the U.S.?
Measles is extremely contagious, requiring about 95% vaccine coverage. Outbreaks happen when local coverage falls below this, allowing the virus to spread among the unvaccinated.
Who depends most on herd immunity?
Those who can’t be vaccinated (due to age or health) or for whom vaccines are less effective—the very young, elderly, and immunocompromised.
Is herd immunity realistic for COVID-19?
It’s challenging because of waning immunity and variants, but high vaccine uptake still greatly reduces severe disease, hospitalizations, and deaths.
What’s the difference between herd immunity and the herd effect?
Herd immunity is the threshold at which outbreaks cannot sustain themselves; the herd effect is any reduction in disease due to vaccination, even if outbreaks can still occur.
Why should I still vaccinate if most others do?
Vaccination both protects you directly and adds to community protection; when vaccine coverage drops, your risk rises—even if others are already vaccinated.


